More than half of adults in the United States have some form of gum disease, also called periodontal disease. Some individuals have inflamed gums, while others suffer from damage to tissues and tooth-supporting bone. If left untreated for too long, periodontal disease will result in tooth loss.
Maintaining dental health makes it easier to ward off other conditions like diabetes and heart disease. Preventing or treating periodontal disease can help protect teeth and gums for a lifetime.
Table of Contents
- Symptoms of Gingivitis and Periodontal Disease
- How Long Can Teeth Last with Periodontal Disease?
- Risk Factors For Developing Periodontal Disease
- Options for Reversing Periodontal Disease
Symptoms of Gingivitis and Periodontal Disease
Healthy gums are pink and firm, and brushing or flossing should not make them bleed. Every day, the teeth accumulate a hard-to-see film called plaque, which contains bacteria. Without proper brushing, this plaque-related bacteria remain on the teeth and can irritate and inflame the gums. Periodontal disease begins at the gums and can progressively affect the supportive tissues and bone.
Gingivitis can occur from bacteria build-up and is the mildest and earliest stage of periodontal disease. It causes symptoms like persistent bad breath, gum redness and swelling, painful chewing, tooth sensitivity, and gum recession that makes teeth appear longer. Gingivitis also makes gum bleed easily. Patients can often reverse early phases of gingivitis with daily brushing and flossing, antiseptic mouthwash, and regular dental cleanings.
Although gingivitis is considered a non-destructive form of periodontal disease, it can progress if it remains untreated. Over time, the accumulated plaque turns into tartar, which only professional cleaning can remove. If tartar builds up below the gum line, it can cause the gums to separate from teeth. The disease can move to the underlying bone and lead to further damage.
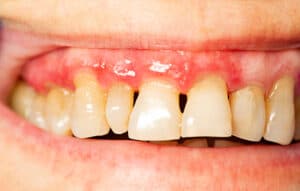
Teeth with Periodontitis
Periodontitis is a more advanced stage of periodontal disease. It occurs when gingivitis goes untreated and infection sets in. It can cause tooth loss, painful chewing, further separation of gums from teeth, bleeding gums, and other health problems. Eventually, periodontitis can break down the gums, connective tissues, and bones supporting the teeth.
Compared to the signs of gingivitis, symptoms of periodontitis can seem more severe. Indications include shifting or loosening of teeth, changes in how teeth come together when biting, pus between teeth and gums, as well as bleeding, and changes in how partial dentures fit.
How Long Can Teeth Last with Periodontal Disease?
Gingivitis can start small and seem unnoticeable at first, but it can manifest as gum inflammation and other uncomfortable symptoms. Over time Stress is a major factor in susceptibility to periodontal disease due to it’s ability to suppress the immune system. Age or disease may also, patients may experience widening pockets between the gums and teeth and destruction of the bone underneath. Although each patient is different, advanced and untreated periodontitis can eventually lead to tooth loss.
Loss of teeth is just one complication of periodontal disease. The damage-causing bacteria can also enter the blood via the gums and affect other body parts. There is a connection between periodontitis and other health conditions like diabetes, coronary artery disease, and respiratory disease.
What Are Risk Factors For Developing Periodontal Disease
- Stress – Probably the most important risk factor. It can be physical stress such as teeth grinding or emotional stress that affects the body’s immune defenses.
- Smoking or Chewing Tabacco – Major Risk Factor
- Poor Oral Hygiene
- Systemic Disease: Such as Diabetes or Immunocompromising Disease
- Malnutrition
- Pregnancy
- Cancer Therapy
- Medication
- Obesity
Options for Reversing Periodontal Disease
So can you reverse periodontal disease? Patients with milder cases of gingivitis can learn how to reverse periodontal disease with proper oral hygiene at home. If gingivitis does not go away or develops into periodontitis, some form of dental intervention will likely be necessary.
Some treatments include initial care by a dentist and follow-up treatment at home. For instance, a dentist might recommend scaling and root planing. Scaling involves removing the tartar below the gum line and root planing smooths over the roots’ surfaces so that the gums can reattach to the teeth. This dual procedure removes bacterial deposits and allows the gums to heal. Depending on the extent of the damage, scaling and root planing may require more than one dental appointment. Patients might need follow-up visits to monitor and treat reoccurrences.
Some patients with advanced periodontitis might need the help of a dentist who knows how to shrink gum pockets. Surgical pocket reduction or flap surgery removes tartar from the gaps. The surgeon also lifts the gums to clean thoroughly underneath them before suturing them. This procedure reduces or eliminates the pockets and prevents future infections. When insufficient amounts of the gums exist, a dental surgeon can perform a gum graft to regenerate the missing tissue.
Surgery cannot repair some advanced periodontitis cases, which is when tooth loss usually occurs. In such cases, patients can opt for dental implants to restore their smiles and everyday functions like talking and eating. Implants look natural and can last a lifetime with proper at-home care and regular dental check-ups.
In addition to surgery, prescription medication can provide relief and treat advanced periodontitis. A dentist can deliver antibiotic or antimicrobial medicine to target the bacteria and slow the progression of periodontal disease.
Although many individuals can learn how to reverse gum disease, the best treatment is prevention. Maintaining a consistent routine of daily flossing and twice-daily brushing with an electric toothbrush can go a long way toward preventing periodontal disease and subsequent tooth loss. Individuals might also incorporate regular rinsing with an antiseptic mouthwash. Eating a healthy diet and getting regular dental check-ups should also be part of an oral hygiene regimen.
- Dental Implant Pros and Cons - August 26, 2023
- Receding Gums Stages - August 12, 2023
- When Is It Too Late for Gum Grafting? - July 8, 2023


